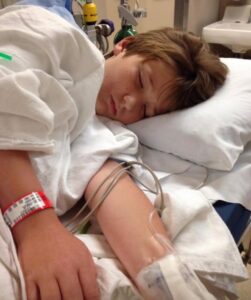
From Marianne Banister: our Claire Marie Co-Founder, CEO, and Claire’s Mom
We are now approaching our 12th Christmas without Claire. It never gets easier.
Rarely do I reveal the work we do behind the scenes at the Claire Marie Foundation. We love to share all the fun stuff; the excitement of our programs and events on our social posts. But because this is an extremely challenging time for nonprofits everywhere, so I wanted to pull the curtain back a bit, in the hope you will better understand the mountains we must climb.
As you know, at the Claire Marie Foundation, our focus is on preventing melanoma in adolescents and young adults through education, awareness and advocacy. We do not spend our funds on research and treatment post-diagnosis; not because those are not important avenues to beating cancer, but because we discovered prevention is overlooked and the easiest solution. In short, if you can prevent a cancer before it develops – there is no need for treatment. 
Having said that, when needed, we step up to join in the good fight for melanoma research funding and to gain access to trials and treatments for younger patients who are refused access or pushed aside. The thought is – kids aren’t at significant a risk, so let’s focus on adults.
True, children, adolescents and young adults do not get cancer as often as our older population. But if you want to see the Mama Bear in me come out, just suggest melanoma is “rare” in young people. It is absolutely is not. In fact, national studies show diagnosis is at “epidemic” proportions in those under 30 years. Plus, melanoma is more aggressive and invasive in young people so effective diagnosis and treatment is essential to survival. To clarify; while the number of overall young patients is not as high as older adults, the risks are greater. And in the experience of anyone who has lost a child, the impact is unimaginable; to the parents, siblings and general community. It is a loss of hope and a future filled with endless possibilities. 
This year, 2025, has left us all reeling with massive federal cuts to cancer research for the National Institutes of Health and the National Cancer Institute. Research grants have been terminated, clinical trials have slowed, and, in some cases, have been brought to a screeching halt. There have been staff layoffs, and long-term projects with new life-saving findings jeopardized, if not completely eliminated. As research is impacted, so too is funding that trickles down to advocacy organizations such as the Claire Marie Foundation. Prevention, research and treatment all work hand-in-hand.
This past summer, as the Co-Founder and CEO of the Claire Marie Foundation, and what is called a “Melanoma Mom”, I was asked to join a coalition of melanoma nonprofits in the fight to correct a ridiculous ruling by the FDA, which in essence signed a death warrant for those with late-stage metastatic melanoma. To set the scene, think of the Peanuts cartoon where Lucy yanks the football away from Charlie Brown just as he’s about to victoriously kick it! Dr. Vinay Prasad, an RFK Jr. appointee, was “Lucy”.
In a surprise, 11th-hour move, he blocked FDA approval of Replimune’s RP1 after it had checked each of the FDA’s required “boxes” in the drug trial process. RP1 has proven to be the Holy Grail of late-stage melanoma treatments for patients who typically have little chance of survival. His decision, with little explanation, blindsided researchers, trial investigators, and patients who were thriving on the treatment. All this halted access to the therapy, which was saving lives.
Given the massive public outcry and advocacy from the Claire Marie Foundation, along with melanoma powerhouses such as AIM at Melanoma, Melanoma Research Alliance, and Melanoma Research Foundation, I am happy to report that the FDA is now reconsidering the approval of RP1. If all goes well, by April of 2026, RP1 will be fully available to those who need it most, offering hope that they may reach a point in their lives where they can live fully with NED, “no evidence of disease”.
All I could offer in my role as CEO, and more importantly, as Claire’s mom, was some insight into the challenges she faced when fighting to get access to trials that could have saved her life. It was a different battle in 2011 when very little was understood about adolescent melanoma, and it was nearly impossible for a person under 18 years of age to gain access to life-saving trials. We are proud that, by sharing Claire’s story over the years, we have pried the door open – just a bit – to allow access to drug trials for those under 18. Still, one thing that hasn’t changed: treatment delays of hours, days, and weeks cost young lives. Patients and their families invest significant hope and financial resources in participating in a trial. There better be a damn good reason to yank it all away. No one deserves to be Charlie Brown. Not my daughter. Not any other young person fighting the good fight. Below is the protest letter I sent to the FDA as part of this summer’s campaign. It is proof that, even though our world is chaotic and hope can sometimes dim, there is still great power in standing up, standing strong, joining forces, and speaking out for what is right.
To: U.S. Food and Drug Administration
From: Marianne Banister Wagonhurst / Co-Founder / CEO / Claire Marie Foundation
August 1, 2025
This October 16th will mark 11 years since we watched our beautiful 17-year-old daughter Claire Wagonhurst succumb to the brutality of adolescent melanoma. No one could prepare us for the emotionally and mentally shattering effect of watching our child take her last breath, knowing it all could have been prevented had she been granted access to life-saving drug therapies.
An athlete, artist, and vibrant young woman, we could only watch as Claire withered away, becoming blind and immobile, a mere shell of herself. Claire would most likely be with us today had she been granted access to trials for one of two drugs, both of which have now become routine in melanoma care: Opdivo and Keytruda. Despite campaigns on her behalf by her oncologist at Johns Hopkins and Senator Barbara Mikulski of Maryland, Claire was denied access because she was not yet 18. Her teenage body was mere months away from that of a “full adult” in trial terms, but the answer was still no.
Ironically, a few months later, after Claire’s melanoma had advanced to her brain with leptomeningeal disease, Keytruda was approved in July of 2014. Claire was one of the first in the country to gain access to the drug; her age was no longer a factor. Our oncologist was excited, deeming Keytruda’s impact significant and even “miraculous”, but it came too late. Too late. Too late. Much, much too late. Claire passed three months later.
Our family established the Claire Marie Foundation in honor of Claire, with the mission of preventing melanoma in adolescents and young adults. It is a population ignored and misunderstood by the medical community, even though melanoma is statistically at “epidemic proportions”. Melanoma is the second most common cancer in adolescents. It is the number one cancer in young adults under 30. It is the most common cause of cancer death in young women aged 25-30. And, as in Claire’s case, it can be triggered by hormonal changes of puberty and even pregnancy. But what is essential to understand when it comes to the topic at hand of FDA drug approval is this: melanoma in young people is more aggressive and more invasive than in older adults, per a study by Johns Hopkins in 2014. There is no time to waste.
Allow me to restate more clearly. Adolescents and young adults diagnosed with a Stage 3 or Stage 4 melanoma, cannot wait for the FDA to reboot. Melanoma is an absolute beast in the young body. Replimune’s RP-1 may be the only thing to save them. By changing the rules at the 11th hour, by denying access to this life-saving drug which has been well proven to be safe and effective, the FDA may as well sign their death orders. It is simply an unconscionable and irresponsible act.
I offer a thought for consideration. In the English language, we have a word for someone who has lost a spouse: widow or widower. We have a word for someone who has lost their parents: an orphan. We do not have a word for someone who has lost a child or a sibling. Perhaps because we simply cannot wrap our minds around the concept. It’s too horrifying. Trust me. It is the most unfortunate of clubs. As a leader, may you make the wise decision to grant approval and thus save other young people, parents, siblings, and families from my fate.
Marianne Banister Wagonhurst
 Well, here’s a disturbing thought: One standard drink increases your risk of developing melanoma by about 20%. So, if you drink five beers, you’ve just increased your risk by 55%. Now, make that drink a margarita and you could really be in trouble; at least when it comes to the sun! Medically speaking, it can cause a severe sunburn, better known as a Margarita Burn, or phytophotodermatitis.
Well, here’s a disturbing thought: One standard drink increases your risk of developing melanoma by about 20%. So, if you drink five beers, you’ve just increased your risk by 55%. Now, make that drink a margarita and you could really be in trouble; at least when it comes to the sun! Medically speaking, it can cause a severe sunburn, better known as a Margarita Burn, or phytophotodermatitis.








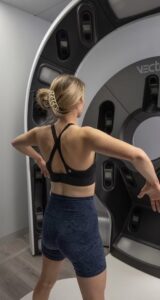
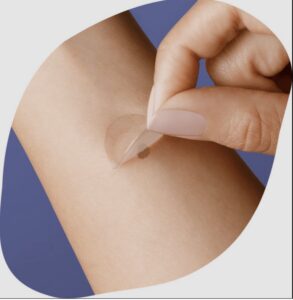
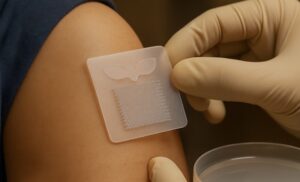 And taking the next step is ExoPatch, currently being tested by researchers at the University of Michigan. This tiny patch has micro needles that capture biomarkers in the top layer of the skin’s epidermis. Researchers say by using this, no biopsy is needed and it can be done at home.
And taking the next step is ExoPatch, currently being tested by researchers at the University of Michigan. This tiny patch has micro needles that capture biomarkers in the top layer of the skin’s epidermis. Researchers say by using this, no biopsy is needed and it can be done at home.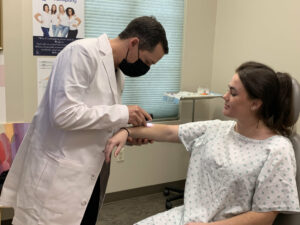

 It often starts in the little ones; as early as 5 years of age. They learn to swing a bat, serve in tennis, pass a football, kick a soccer ball or cradle in lacrosse. Over the years, their time on turf, courts, and grass will increase as will their exposure to the damaging rays of the sun. On average, the NCAA outdoor athlete will spend 1,200 hours a year in the sun. But that doesn’t even account for the years before college.
It often starts in the little ones; as early as 5 years of age. They learn to swing a bat, serve in tennis, pass a football, kick a soccer ball or cradle in lacrosse. Over the years, their time on turf, courts, and grass will increase as will their exposure to the damaging rays of the sun. On average, the NCAA outdoor athlete will spend 1,200 hours a year in the sun. But that doesn’t even account for the years before college.



 This Melanoma May, we turn the spotlight on the guys! New research is focused on the surge in the number of young men
This Melanoma May, we turn the spotlight on the guys! New research is focused on the surge in the number of young men

 Here’s some food for thought: Nearly 400,000 children and adolescents will be diagnosed with cancer globally this year. That means every three minutes, a parent is told their child has cancer. Trust me. No one can imagine nor prepare for the moment. There is simply the before and the after. Life is never the same. Still, there is so much more hope for young patients, since we lost Claire nearly a dozen years ago. That is due in great part to the advocacy and commitment of researchers and to those who scramble to find funding, who make it all happen. But times are hard.
Here’s some food for thought: Nearly 400,000 children and adolescents will be diagnosed with cancer globally this year. That means every three minutes, a parent is told their child has cancer. Trust me. No one can imagine nor prepare for the moment. There is simply the before and the after. Life is never the same. Still, there is so much more hope for young patients, since we lost Claire nearly a dozen years ago. That is due in great part to the advocacy and commitment of researchers and to those who scramble to find funding, who make it all happen. But times are hard.
 Dr. Robyn Gartrell, M.D., a Pediatric Oncologist and Research Physician with Johns Hopkins University School of Medicine, finds frustration in the fact that children are often eliminated from drug trials under the assumption that their systems are too sensitive, and the drug therapies could do more harm than good. In fact, Dr. Gartrell has found that the children can actually fare much better. “I’ll say, children have a higher tolerance and often survive what adults can’t. Case in point is CAR T Cells. Adult patients died from the immune response called cytokine release syndrome and while it is scary in children too, they often survive with fantastic supportive care as their bodies can handle things adults can’t.'” When asked why she keeps fighting the good fight, Dr. Gartrell says it is all about hope: ” Providing a drug to a child with a terminal cancer that allows them to not only plan for but go to college is an unreal feeling.”
Dr. Robyn Gartrell, M.D., a Pediatric Oncologist and Research Physician with Johns Hopkins University School of Medicine, finds frustration in the fact that children are often eliminated from drug trials under the assumption that their systems are too sensitive, and the drug therapies could do more harm than good. In fact, Dr. Gartrell has found that the children can actually fare much better. “I’ll say, children have a higher tolerance and often survive what adults can’t. Case in point is CAR T Cells. Adult patients died from the immune response called cytokine release syndrome and while it is scary in children too, they often survive with fantastic supportive care as their bodies can handle things adults can’t.'” When asked why she keeps fighting the good fight, Dr. Gartrell says it is all about hope: ” Providing a drug to a child with a terminal cancer that allows them to not only plan for but go to college is an unreal feeling.”